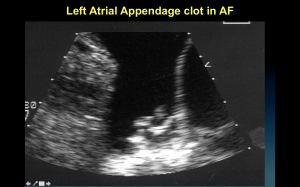
When it comes to the risk of stroke in atrial fibrillation, it pays to be a boy. Sorry, ladies.
An important question came up on my recent post on AF and stroke.
Why does being female give you an automatic point on CHADS2-VASc? I keep seeing it, but I don’t see why that is.
It doesn’t seem intuitive that female AF patients should have more strokes. Why? AF should equal AF.
But it does matter. When it comes to AF and stroke, women are very different.
Here are three references that support the fact that female gender increases the risk of stroke in AF.
–First: This Italian study of 780 AF patients on blood-thinners, published in the British blood journal, Thrombosis Haemostasis, reported three main findings:
- Female gender did not increase the risk of bleeding.
- Female gender—even when correcting for age–doubled the risk of stroke.
- Females had more disabling strokes, including a three-fold greater risk of fatal stroke.
–Second: From the British Medical Journal (January 2011): This registry-based look-back Danish study of more than 70,000 AF patients between 1997-2006 showed that female gender alone increased the risk of stroke. Additionally, adding female gender with other moderate risk factors (high blood pressure, age > 65 and vascular disease) greatly accentuated stroke risk. It was a strong study due to the huge number of subjects.
–Third: The strongest study to date on gender-related differences in the risk of stroke in AF comes from the ATRIA study, published in 2005 in Circulation. Researchers form California and Boston looked back at more than 13,000 AF patients. They found that females had a 60% greater risk of stroke. The enhanced risk occurred at all ages and held up after correction for confounding diseases. Reassuringly, they also found that warfarin reduced stroke risk equally in females and males.
Data like this is why European AF specialists believe that female gender warrants a point on the CHA2DS2-VASc score.
AF patients and treating docs have to remember that stroke represents a devastating complication from AF. There exists many situations where one can live reasonably well with partially damaged organs; the brain is often not one of these. Sight, memory, speech, cognition, ambulation, and continence are all brain-controlled functions that directly relate to quality living. Stroke is to be avoided. And another thing to think about: though bleeding is a risk of blood thinners, bleeds rarely leave permanent damage. Bleeds can be treated and often are impermanent–unlike stroke.
Here are the pertinent risk factors for stroke:
C: Congestive Heart Failure (or a weak heart muscle; low ejection fraction)
H: High Blood pressure
A*: Age above 75
D: Diabetes
S*: Previous stroke or TIA (or clot)
V: Vascular disease (CAD, PAD, Aortic plaque)
A: Age between 65-74
Sc: Female gender
The data is clear; if one or more of these risk factors are present, the evidence strongly suggests thinning the blood with either warfarin or dabigatran protects one from stroke.
Hope this helps.
JMM
* – Represents very strong risks and warrant two points on the CHADS-VASc scoring system.
4 replies on “Female gender and stroke risk in atrial fibrillation: Know your CHA2DS2-VASc Score”
Dr. Mandrola,
Thanks for the great article. It’s always bugged me that CHADS2 fails to consider women’s greater stroke risk, which is why CHA2DS2-VASc was such an improvement when it was introduced a couple of years ago.
I often remind women with afib that over 60% of stroke deaths in the US are in women (according to American Heart Association). You can bet that a huge portion of those are due to afib strokes since afib strokes are 3 times more fatal in the first 30 days than other strokes, and 2 times more fatal overall.
What I think is particularly sad is that while patients are more scared of stroke, many doctors are more scared of bleeds (acts of commission rather than omission), and thus many females, especially elderly, do not get anticoagulants. How can we solve this problem?
Mellanie
If the high blood pressure is controlled by medication is it still a risk factor? Also, in females of higher age, if the afib has been successfully ablated, is anti-coagulation still called for?
Good questions.
On BP, most feel that medically-treated high BP still counts. On ablation, unless AF can be documented to be cured–those with pacemakers, implantable recorders or long-term monitors–the recommendation for post ablation blood-thinning is the same as pre-ablation: per CHADS-VASc score.
I don’t smoke, I excercise regularly, I eat right (at least try), I don’t drink much (maybe I should), I’m under 65, and I take my warfarin every day like a good girl. Did I say “Girl”?…OMG! What do I do?
You really don’t have to answer that.
Thanks for the pick-me-up Doc!
All joking aside, I truly believe knowledge is power. Seriously, thanks for sharing your valuable insights on AFib!