AF News Flash:
Heart surgeons are on the case!
An important trial comparing catheter ablation to surgical ablation for AF was reported at last month’s AHA meeting. The surgical ablation arm of the FAST trial used the newly-approved Atricure Synergy Ablation System.
And onward goes the collegial tussle between heart doctors and heart surgeons.
Before speaking about surgical ablation of AF, let me offer a prologue on the intersection of heart surgeons and heart doctors.
My career in cardiology has seen heart doctors gradually migrate onto the playing field of heart surgeons. First, we started squishing, then stenting, blockages that were once only bypassable. In the rhythm world, surgeons led the way in pacing and defibrillators. Then, when technology made devices smaller, heart rhythm specialists became the installers. Surgeons led; heart doctors followed.
In the case of AF ablation, the order has been reversed. Heart rhythm doctors from Bordeaux first described using a catheter to ablate AF. And so began the era of electrically-isolating pulmonary veins and AF ablation. More than a decade later, AF ablation dominates the practice of many heart rhythm specialists, like myself.
Now however, with the FDA approval of Atricure’s Synergy Ablation System, heart surgeons, their caseloads diminished by interventional cardiologists, see the opportunity that is the epidemic of AF. Medical device companies also see the opportunity. They know that heart doctors (who possess the skill-set for AF ablation) can’t possibly ablate the millions with AF. So they are making tools not just for us, but for surgeons too.
What is surgical ablation of AF, and how successful is it?

A few enterprising surgeons, usually from single centers, have pioneered a different way to treat AF. Unlike catheter ablation, surgery for AF approaches the heart from the outside (epi-cardial). This requires making incisions on the chest. Early reports of the Maze procedure, from Dr James Cox in St Louis, involved using a cut and sew technique on the atria. This challenging procedure requires sawing the sternum and using heart-lung bypass.
More recent iterations of surgical ablation–dubiously termed minimally-invasive–approach the heart through thorascopic incisions in both chest walls. These mini-maze procedures use the Atricure device to electrically isolate the PVs, make lines of block and ablate neural inputs to the atrium.
The good news about surgically-made lines are their durability. Surgical lines, which are delivered under direct sight of the operator without radiation, seem to more reliably create complete (transmural) lesions.
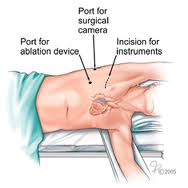
Mini-mazes, however, should not be confused as all that ‘mini.’Â Patients are exposed to lengthy periods of anesthesia, sequential deflation of the lungs, chest wall access (painful) and dissection of important structures in the chest. And like catheter ablation does, these procedures require hard-won surgical skills, honed over many cases. They are not easy.
AF Surgery Results?
AF surgeons are known for their amazing reports of success. Some brashly report over 90% success! The problem is these results are often either unpublished or are single-center, non-controlled series with short duration and lax follow-up. Heart doctors also cite concerns that more extensive surgical ablation may permanently alter the squeezing function of the atrium—thereby increasing stroke risk. On stroke risk, surgeons counter that they can excise the left atrial appendage—a frequent source of blood clots.
Surgeons would also–and rightly–cite important limitations of our catheter-based ablation procedure:
- it’s technically demanding, requiring an incredible degree of human deftness, gained only through performing many procedures over years.
- single procedure success is less than ideal–around 50-60%. Even the best centers report the need to do multiple procedures.
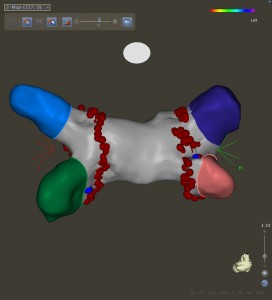
- Most often, recurrence of AF after catheter ablation occurs because the point-to-point ablation lesions (imagine drawing a line with dots) develop gaps. Other times, the lines of block hold, but the driver of AF resides elsewhere (think isolating Maine, Florida, Seattle, and LA, but AF comes from Kansas.)
- Even in skilled hands, the procedure has significant risks: puncturing the heart, stroke, stenosis (blockage) of pulmonary veins and the most-feared, esophageal damage.
- And efforts to increase the success rate of AF ablation have met resistance. Doing extra burns, outside of just isolating PVs, frequently results in atrial flutter, which can be peskier than AF. Newer technologies, like expensive robots, cryo-balloons, and lasers have not (yet) made the procedure safer, easier or more effective.
Until the FAST trial was presented at last month’s AHA meeting, there wasn’t any evidence base comparing the two strategies in a head-to head study. Though FAST enrolled small numbers of patients from only two European centers, it is an important study because it directly compares two competing approaches, for the first time.
(Before addressing the particulars of the trial, it’s important to say that most surgical ablation of AF today occurs at the time of heart surgery for other reasons–valve replacement and bypass. The FAST trial addresses stand alone AF surgery.)
Researchers from Spain and the Netherlands enrolled 124 patients with medically-resistant AF to undergo either a catheter ablation or surgical ablation using the Atricure device. Patients had enlarged atria and more than two-thirds had failed prior catheter ablation. Freedom from AF (just 30 seconds) was the primary endpoint. Seven-day monitors were used at 6 and 12 months.
Results:
Surgical ablation worked 65% of the time versus only 36% for catheter ablation. Allowing for the use of AF meds after the procedure improved success rates to 78% for surgery and 43% for ablation. But the improved results of surgical ablation came at a cost. Surgery caused many more serious adverse events: 34% versus 15%. Surgical patients averaged 5.5 days in the hospital versus 2 days for catheter ablation. Most of the adverse events in the surgical arm related to getting access to the heart from the chest wall.
My comments on the FAST trial:
1. The catheter ablation procedure used in FAST was flawed.
In one of the two centers, the (non-irrigated) ablation catheter used is outdated and considered less effective. Also, patients ablated with a catheter underwent “extra lines placed at the discretion†of the operators. These extra burns are thought to increase the procedure’s success, but many experts think they actually lower the success rate—by increasing the chance for atrial flutters. (Researchers even stated that in some cases, conduction block across the lines was not confirmed. It is known that creating partial block can make the rhythm worse.)
2. Patient selection stacked the deck against catheter ablation.
Enrolling large numbers of patients that failed catheter ablation and with large atria may favor surgical ablation because more advanced states of AF are tougher to ablate with a catheter. This line of reasoning is strengthened by the very low rates of success in catheter-ablated patients–36% is far below most published reports.
3. The endpoint was defined unrealistically.
Many regular AF doctors might say the endpoint, freedom from just 30 seconds of AF, was overly strict. For instance, few clinicians and patients would call a 1-minute run of silent AF a failure. It might have been more telling to look at longer runs of AF as the endpoint.
In summary, the researchers deserve praise for this important contribution. The bottom line in FAST was that surgery bested catheter ablation for suppressing AF, but was associated with a high (one in three) rate of serious adverse events.
These data highlight the difficult decision of treating AF, a non-life-threatening but highly bothersome disease, with very aggressive means.
The struggle to triumph over AF continues. Heart surgeons are adding to the knowledge base of AF. This is good. AF patients should be glad they are on the case. I am.
Stay tuned. There is surely more to come.
JMM

5 replies on “Surgical versus Catheter Ablation for Atrial Fibrillation”
Can the two approaches be complementary? As a patient, my treatment has progressed from medication to electrocardioversions ( 7 of them) to catheter ablations (3). Would not surgical ablation be the next logical step in the progression should another intervention be needed?
Yes Don. I send a small number of difficult cases each year for consideration of surgery.
I continue to be very appreciative of the information you provide on your blog, Dr John. It’s helped me gain much insight into the new world I was thrust into.
“see the opportunity that is the epidemic of AF”
Do you see the rising cases of AF as a true increase, or just better diagnosis and screening?
Any comments as to why the cases may be increasing, if they indeed are? I suspect it follows the same general causes of increased heart problems in general. I also wonder seriously about the huge changes in our social fabric that may play a part. With modern technology, unless you REALLY work at it, you can never get away from the constant cellphones, emails, texting and general nuisances that others expect you to respond to. “I sent you a work related email while you were on vacation, and you didn’t respond for 20 minutes.Where were you?”. I watch much younger people than me hiking with an mp3 player in their ears, texting and tweeting, surfing the internet, and “enjoying nature”. Talk about instant ADHD! What are they setting themselves up for in the future? Maybe I’m just becoming an old curmudgeon. Sigh . . . . . .
The incidence of AF is clearly on the rise. The most obvious cause relates to the spread of obesity and its effects: high blood pressure, sleep apnea and coronary heart disease, to name only a few. As AF is a disease of aging, that people live longer–but perhaps not better–also contributes to the spread of AF.
On your point about an inflamed over-scheduled populace, I commend you on reading between the lines of my posts. My anecdotes are adding up to a narrative. Why, I ask, does a steady stream of successful CEOs, lawyers, doctors, engineers (lots of engineers) and even seemingly hyper-fit athletes keep turning up in my office with AF? These patients all share a common bond: they are mostly over-achieving, over-worried, self-absorbed and some might say, inflamed.
AF is defined by its diversity, its vastness and its unpredictably. There are few rules.
But still, I see two repeating phenotypes of the AF population. Call them dominant frequencies, if you will. There are the aging patients with high blood pressure, high body fat and sleep apnea. These patients have the ‘classic’ risks factors for AF. On the other side of the spectrum are the over-achievers. They are intellectual, thin, fit, over-worried and mostly over-scheduled. Is inflammation the common bond? Some are inflamed by doing too little and the other by trying to do too much.
And what role do genes play? Clearly we are learning that AF often has a genetic basis. I wonder whether people not only inherit specific electrical abnormalities that cause AF, but also the personalities that foster AF.
Gosh, I better stop.
Thanks for the great comments.
Dear Dr. John,
Thank you for your review of the FAST study and your willingness to debate these important issues on your blog.
The FAST study is the first head-to-head comparison between the catheter based and a surgical approach. It is a very courageous study both from the surgeons who did the surgical cases and the electrophysiologists who participated in the study. It also has very high quality standards and both procedures were held to the same standards.
From my perspective the study documents without any doubt that catheter ablation is far less effective than surgical ablation. This is inherent in the two approaches as “connecting the dots†have to be less effective than multiple solid epicardial ablation lines. In addition, the surgeons used stringent quality assurance routines by pacing across the ablation lines to verify electrical block.
I agree that there is a higher procedural complication rate in the surgical group. However, the surgeons honestly documented every possible complication including mild pneumothorax (which were around 50% of the procedural surgical complications).
In your review you do not comment on the long term severe adverse events. The catheter ablation patients experienced one stroke, one TIA, two heart failures and one death. No patients in the surgical group experienced these severe long term complications.
The FAST study is a real challenge to the electrophysiologists: they need to improve their procedures, the procedural quality assurance methods and the honesty in documenting outcomes. I would team up with the best surgeons in your community and take the time to learn together. The solution to AF treatment lies in a cooperative approach between electrophysiologists and surgeons – not trying to pitch this as a “competition†or keeping the door to surgical procedures shut. This will hopefully serve the patients who need improved care (see the comment by Don above).
Jon
Disclaimer: I’m a previous employee of AtriCure