It’s been awhile since I have written about the treatment of atrial fibrillation (AF).
I would like to remedy this by sharing a few thoughts on three recent stories about AF: one involved a soon-to-be-approved blood-thinning drug; the second highlighted a potentially exciting new device for ablating AF, and the third story irresponsibly sensationalized the risks of taking the heart rhythm drug, flecainide.
First the blood-thinner story:
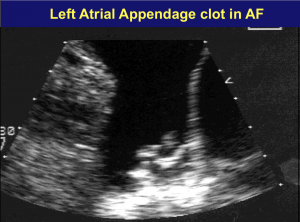
The most devastating complication of AF is stroke. Blood clots that form in the swirl of the non-contracting (fibrillating) atria increase the risk of stroke. Until late 2010, the mainstay of reducing this risk meant taking the dreaded blood-thinner, warfarin (Coumadin).
This paradigm changed, however, when Boehringer-Ingelheim brought us the novel and robustly vetted blood-thinner, dabigatran (Pradaxa), in 2010. Not only is dabigatran more effective in preventing stroke, it is also far more convenient. AF patients that take dabigatran are no longer encumbered by frequent INR monitoring. There is no fretting over how many servings of green vegetables one eats. And finally, dabigatran overcomes this major barrier: nobody’s Aunt or golfing buddy has bled to death on dabigatran—like they did on warfarin.
As of this writing, dabigatran has a monopoly on the non-warfarin oral blood-thinning market.
But not for long…
The financial market for novel ways to treat AF is huge. Heart disease remains our number one cause of death, and AF is the number one heart diagnosis. As a disease of wear-and-tear, AF has flourished in the Western world’s sea of inflammation—a sea overrun by over-scheduling, sleep-deprivation, lack of daily exercise, and abysmal nutrition.
So it is no surprise that pharma companies are developing competitors to dabigatran. This week, we heard news about the next chapter of oral blood thinners. (Interestingly, the story came in the form of a press release from a drug company, rather than a scientific study.)
Apixaban—the next approved blood thinner?
Larry Husten from Cardiobrief, and Shelley Wood at TheHeart.org have nice summaries about apixaban, which Bristol Myers Squibb and Pfizer will call, Eliquis.
This week’s press release reported that in the Aristotle study, which looked at 18,000 AF patients randomized to either 5 mg twice daily of apixaban or warfarin, apixaban was non-inferior to warfarin in stroke prevention and superior to warfarin in a composite secondary endpoint, which summed all types of stroke, bleeding and mortality. The detailed scientific data on Aristotle will be released later this summer at a European Society of Cardiology meeting in Paris.
As Larry Husten rightly says,
“the blood-thinner marketplace may soon get crowded. In addition to warfarin and dabigatran (Pradaxa, Boehringer-Ingelheim), Johnson & Johnson is seeking approval for the [once-daily] rivaroxaban (Xarelto).
Look for a number of questions to emerge when these new blood thinners gain FDA approval.
One will be on efficacy. Dabigatran (a direct thrombin inhibitor) boasts strong data suggesting superiority to warfarin, whereas apixaban and rivaroxaban (Factor Xa inhibitors) have only non-inferiority claims. Is this related to the fact that they block the clotting cascade at a different place? Are they clinically relevant differences? Will there be head-to-head comparisons of each of these agents?
Second will be the value of once-daily dosing (Rivaroxaban) versus twice daily. Doctors on the front lines of treating patients will tell you that once-daily regimens improve compliance. And compliance is a critical issue here because doctors have no means to confirm whether a patient is taking the blood-thinner as directed. Essentially, dabigatran-treated patients are on the honor system. For example, I haven’t recommended switching to dabigatran in all my warfarin-treated AF patients. One of the main reasons for not changing has been my gut-feeling about a patient’s ability to comply with the twice-daily dosing.
The third comparison will center on the side effects of each drug. After six months of using dabigatran, I can comfortably say that GI side effects are common–stomach pains (reflux-like) occur in at least ten percent of patients. Though the belly discomfort resolves with stopping dabigatran, dealing with the problem is an inconvenience for both the patient and doctor. It requires extra time, extra consternation, and perhaps some risk in overlapping blood thinning drugs. If any of the new agents are easier on the belly, look for it to shoot ahead in market share.
Finally, the optimist in me wants to believe that competition might drive costs down. But I am a realist, and this is US health care.
Look for a hearty debate to unfold.
JMM
9 replies on “An update on AF: New blood thinners”
Good piece.
But you make no mention of how these new drugs will be monitored for proper dosage (both at the onset of taking one of the drugs, and then on a continuing basis).
If not INR……….. what?
Thanks for the kind words.
There is no need for monitoring because of the reliable blood-thinning effect of the non-warfarin blood thinners. I have touched on this on other dabigatran posts.
Interesting, but perplexing. It’s hard for me to imagine that “one size fits all” is the case fo0r dosage of dabigatran.
Let me say, again, your blog and comments help enormously in unraveling the mysteries of this affliction for this long-time patient.
I was part of an Apixaban clinical AF study for about a year. When that study was completed I was on Coumadin a short while, then 4 months ago I started medicating with twice a day Pradaxa. I have had no stomach problems since I started Pradaxa. I have been checking into a hip replacement operation, but I am leery of going off Pradaxa for fear of a stroke. My doctor does not believe in bridging with Heparin. Your thoughts?
That’s a question for you and your doctor. “Bridging” with blood-thinners is very case dependent.
I have been advised that Pradaxa and how it works in the clotting cascade may present severe problems in managment of Truama patients on this medication. I was told the difficulty in reversing the effects are more complicated than in a warfarin patient. I notice that in advertisment of the medication it is carefully overlooked. Any suggestions or comments to this?
It is true that there is no antidote for dabigatran. It’s blood-thinning properties cannot be immediately reversed. (Though I am told work is underway on an antidote.)
But practically speaking, this is not likely to be a major clinical issue. For three reasons:
1. The blood-thinning effects of dabigatran wear off in a matter of hours–not days like warfarin. In fact, in all but the most serious trauma centers, in the time it takes to get warfarin toxicity reversed, dabigatran’s effect would be waning.
2. Unlike warfarin, dabigatran does not cause the blood to become “super-thin.” Absent an overdose of course.
3. The 18,000 patient RE-LY trial did not show any major differences in bleeding, nor mortality with dabigatran.
thank you for your insight Dr.
I am a fellow Louisvillian who has been in permanent A-fib since 2003. Took warfarin all of this time except for 3 years I was part of a study either taking apixiban or warfarin. Have been on Pradaxa since March 2011. Tolerating it well.
Thanks for your informative blog.