 It finally happened. After years of sitting at John’s bedside through multiple serious bike crashes, I had one of my own. I’ve had plenty of time to build up a ridiculous amount of smugness about why he crashes and I don’t. “John is reckless; Staci is cautious. John rides like an airplane engine on a shopping cart; Staci uses her head.â€
It finally happened. After years of sitting at John’s bedside through multiple serious bike crashes, I had one of my own. I’ve had plenty of time to build up a ridiculous amount of smugness about why he crashes and I don’t. “John is reckless; Staci is cautious. John rides like an airplane engine on a shopping cart; Staci uses her head.â€
I was mountain biking in Cherokee Park. A storm front was moving in so the temperature and humidity were dropping and it was breezy. I felt so good! Like Rose and Jack on the bow of the Titanic. I was queen of my body and that trail. I passed a real mountain bike racer and I said to myself, “Yeah, I’m a racer too.†Twenty seconds later, my front wheel hit a stick in the trail. My wheel went left and my body went right. My right hip hit the trail and a bolt of lightning lit up my hip socket. I pulled myself to the trail side and checked around. Nothing else hit, no skin lost, no head trauma, nothing. I stood up. Left leg works…right leg does not. Time to go to the hospital.
Now for the observations:
1. Thank goodness for the kindness of strangers. A woman and man found me trying to stand up unsuccessfully. They and a lone mountain biker helped me up a 100-yard grassy slope to the road. The real mountain bike racer came back and wanted to fetch his car and take me to the ED. I waved him on. No sense screwing up two perfectly good rides.
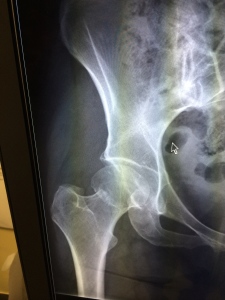
2. It can be fun when you don’t look like the typical person with your diagnosis. After the lightening bolt of pain subsided, my hip really didn’t hurt that badly. I could even move it around some, especially if I was in charge of the moving. The ED doctor wanted to do an x-ray but I don’t think he expected to find anything. It was amusing to watch John and three ED docs look at the x-ray in another room and then look through the window at me with surprise. I already had my answer when the radiology tech said I needed a chest x-ray. All the ED staff were kind to me before and after they knew I had a broken hip.
3. Anyone who touches pee, poop, vomit, sputum or blood without making an eww face is an angel to be thanked at every opportunity. During my first hospital day, I could only lift up on a bedpan to pee. The CNAs, RNs and John assisted me with kindness. I teach medical students, medicine residents and palliative medicine fellows that they must be present with any misdeed the human body, mind or soul can manifest and not make an eww face.

4. Pick good people to care for you and then trust them to do so. John’s orthopedic surgeon is in his list of favorite contacts. She is smart, talented, experienced, compassionate, and a “master of the obvious.†She answered John’s call from the ED, looked at the x-rays and recommended a surgeon who was trained in doing a total hip replacement from the front rather than the back. This meant no cutting through my butt muscles and a faster recovery time.
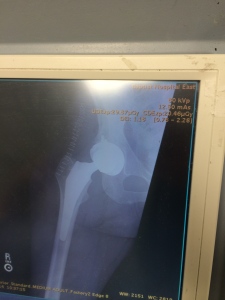
5. I wanted a surgeon who was smart and a good human being. I was pleased to hear multiple physicians affirm that I had picked the right surgeon for my problem. But the deal was sealed when two former OR nurses who had worked with him said he treats everyone with respect, equality and kindness.
6. Healthcare workers freak out when you talk about end of life care preferences. I told one of my nurses if I had a catastrophic complication related to my hip fracture or surgery that necessitated total care or permanent artificial nutrition/hydration, my goals of medical care would change to comfort only. I would want to be allowed to die naturally. Her body shivered and she said I shouldn’t talk about such things. Hip fractures are not benign. If you are an older woman, you have almost a 1 in 10 chance of dying in the first month. Talking about death in this situation is practical. I was able to use a wheelchair independently on my second hospital day so I visited with the RN in charge of palliative services a few floors below my room. I told her my predicament. She knows I have a completed living will declining life prolonging care in certain scenarios. John is my healthcare surrogate. She said she would be available to support John in carrying out my EOL care preferences if the need arose.
 7. Sweet words matter. I care for actively dying people. When I am at their bedside, I tell them things that I would want to hear in the hours and days before death. “I am here… You are safe… You are surrounded by people who love, care for and honor you… I will be here as long as you need me.†I don’t know if these words help; dying people can’t tell me. My anesthesiologist said similar things to me when he was putting me to sleep. I will keep saying my words.
7. Sweet words matter. I care for actively dying people. When I am at their bedside, I tell them things that I would want to hear in the hours and days before death. “I am here… You are safe… You are surrounded by people who love, care for and honor you… I will be here as long as you need me.†I don’t know if these words help; dying people can’t tell me. My anesthesiologist said similar things to me when he was putting me to sleep. I will keep saying my words.
8. Take your pain meds after surgery. I thought I was superhuman since my broken hip seemed nearly painless. I refused the RN’s offer of medication. I treat pain crises often. Until I had my own, I did not comprehend how trapped inside your miserable body you feel. I did not escape until hours later when the opioids kicked in. (Editor’s note: Please note that she did not call them narcotics.)
9. Take your laxatives. Pooping is imperative.
10. Have good family, friends and coworkers. All the calls, texts, visits, and care packages were so appreciated. Catherine is my right leg woman at home. Will is my sane perspective. Charlotte is my joy. And John. He sat by my side, coordinated my care, helped me pass the time and worried about me when I was gone from him. Thank you and I love you endlessly.
SAM
Disclosures: The only thing I promote is good palliative care for people who seek my advice. I did have free and easy access to many physician colleagues for their expert opinions. As the perks of being a physician dwindle, I will happily claim this one.
22 replies on “Guest post — 10 observations from a 49 year-old falls risk.”
Staci –
So sorry to hear about your accident! I hope you (and John) have an uneventful recovery. No doubt you’ll be back on your bike, perhaps with a new appreciation for the wonder of this human machine and the wonder of medicine, in short order.
God speed.
-Wes
Great post! Thank you both. Staci, I had bi-lateral hip replacement 14 years ago – before I started riding my bike. You will be back in the saddle in no time! Now if only I could shake this dadgum AF!
Best of skill to both of you!
SK
Glad to hear you’re on the mend, Staci! I’ll keep you and The Fam in my thoughts and prayers!
Life is good
Murphy
I am a 78 year old woman with congestive heart failure, COPD, Afib. 4 years ago while out for a walk I fell and broke my pelvis in 3 places. Had to crawl some distance in order to get help. All you say is well said. And healing does take place. This weekend I’m going canoeing with my daughter in Minnesota’s Boundary Waters.
Thanks for sharing your story Staci. When clinicians become patients there are lessons for us all to learn. Even if we think we are very patient-centered to begin with. I have seen some of the same experiences as a caregiver for some older members of my family. That experience is also illuminating.
Staci,
I’ve only met you a couple of times but I LOVE your bluntness.
On the bright side, being a biker without a big fall and a broken bone is like being a high school shop teacher with 10 fingers. You just aren’t in the club yet.
Sounds like you are now in the club in a big way!! You can officially nerd out on bike crashes with the most aggressive bikers.
Seriously, glad you are okay.
Dan
Staci – THANK YOU for writing this column! Glad to hear that you got through surgery well and seemed to be healing. I have learned the most about our medical system when I was “the patient”. Had 2 episodes during my family medicine residency (acute total tear of my achilles tendon; testicular torsion at age 26 … ) – it was truly humbling yet fortunate for me that I had good providers and all turned out well. Wishing you THE BEST for speedy recovery!
I’ve just started exploring Dr. John’s blog, but your post strikes a chord as I had a similar fall and injury 20-some years ago when I was about 30; I hit a patch of gravel while road riding and came down hard on my right side, breaking my femur near the hip joint. At the time I was working in the hospital where I had my surgery—rod insertion, so it was an opportunity to see things from the “other sideâ€. The staff overall did a good of making a miserable experience less so.
Anyway, curious if bone density was discussed in your case? There are claims floating around that cyclists in particular are prone to lower bone density. I’d always wondered, as my fall was low-speed and non-violent, though into concrete. But I wasn’t tested until this year, after breaking ribs two years in a row. In calling with results they didn’t quantify it, but said it’s right at the edge of osteopenia, and no treatment was indicated, other than getting sufficient vitamin D and calcium.
The calcium thing is somewhat of a dilemma, as some doctors are saying that supplementation is not worth the possible risk to heart health. Perhaps Dr. John has discussed this already? My thought is that a calcium supplement labeled as extended release might be safer than otherwise.
It’s inflammation… according to this alert:
http://www.medpagetoday.com/resource-center/Osteoporosis/inflammation/a/46130?isalert=1&uun=g42415d2173R5041927u&utm_source=Alert&xid=NL_ALERT_2014-09-19
D plus calcium: a contentious subject.
Is a “sufficiency” of D really enough? Is enough magnesium as essential as enough calcium? Zinc? Boron?
Research suggests that vitamin K2 in the diet effects vascular and skeletal calcium.
I appreciate your comments and link. They reinforce in my mind the vast room for improvement remaining in medical science. Statistical associations are sometimes strong enough to support recommendations for drugs and lifestyle choices, but mainly they tease us with hints of the underlying complexity in the interaction of our genes and environment.
As you imply, vitamin D supplementation is also an issue. In my case, as a result of borderline low blood levels, my PCP has been pushing for a 50,000 IU single dose in addition to something like 3-4000 IU daily. Yet there’s at least the possibility of causation in unpleasant joint and tissue pains that correlated with previous 2000 IU daily supplementation. On top of that, Steven Salzberg argues that vitamin D supplements “are a waste of money,†citing various Lancet articles: http://www.forbes.com/sites/stevensalzberg/2014/01/13/the-top-six-vitamins-you-shouldnt-take/
Apologies to Staci for the divergence. I hope your recovery is going well.
Contentious, oh yes.
The article you cite, on pubmed:
http://www.ncbi.nlm.nih.gov/pubmed/?term=%22Vitamin+D+status+and+ill+health%3A+a+systematic+review%22
Go to “comment in” at the bottom, click on each link, then click on the lead author. Tease out the science…if you can.
Tease out the science? Sorry, I’m just an engineer.
All the better!
So young! You’ve got again as many years to go — now, with a man-made device to carry you there.
Which makes me wonder about materials choices, if I may.
With the “free and easy access to many physician colleagues for their expert opinions”, do you now have state-of-the-art ceramic-on-ceramic, ceramic-on-cross-linked poly, something even better?
Are the implants hydroxyapatite coated?
I hope these ten days or so of recuperation have been good for you. He does the dishes, right?
Glad to hear the happy outcome of your story. One suggestion I’d add is that if anyone is out alone, riding or walking, be sure you have your charged cell phone with you! I fell one early morning while walking my dog; no one was around, I couldn’t walk (at first), didn’t have my phone to call for help, and had to eventually struggle to crawl to my house, while still trying to hang onto the 80 # dog (no Lassie, that girl!). Lesson learned and fortunately, despite the pain, I didn’t break anything! Best to you and your readers.
Wes, Steve, Andy, Marilyn, Christian, Dan and Kenneth!
Thank you for all the well wishes and support. I am a week post-op. I have walked everyday, some days with one crutch, some days with none. Some days it hurts, some days not. I’m planning to get in that canoe with Marilyn within the year!
Jeff-
I am a little fuzzy on the materials used in my hip replacement. I think I have a titanium implant with a ceramic/polymer socket. I don’t think I have a hydroxyapatite coating. I see the surgeon on 9/30 and will get details.
Jonathan and Jeff-
It’s great that you brought up causes and supplements for recovery. I will make another disclosure. I have been a supplement/granola girl for the past 20 years. I skip pharmaceuticals and treat myself with whole food nutrition, exercise and good sleep. I am hitting the program hard after this experience.
I love this PDF by Susan E. Brown, PhD Center for Better Bones 605 Franklin Park Drive East Syracuse, NY 13057 http://www.betterbones.com. It is titled “How to Speed Fracture Healing.” It is well referenced from both nutritional and scientific journals. I have not read and vetted each individual study. That’s the beauty of a DrJohnM post!
I do agree that we over supplement calcium in this country and under supplement magnesium and vitamin D. Prior to this THA, I took daily Vitamin D3, magnesium and Vitamin K2 supplements. Now I have added calcium to this mix as recommended by Susan Brown.
My supplements are all organic and whole food sourced. The calcium I’m using is derived from algae, not seashells. I have no data to support this, but will be on the lookout in the future.
I have not had a DEXA scan. I imagine this will be in my future. I can say the impact was so violent, it would have been a miracle not to break a bone.
I’ll keep you posted on how it all works out. Thanks again for your comments and interest!
Staci, I thought this might interest you — professionally.
http://onpoint.wbur.org/2014/09/23/end-of-life-care-health-care
I wonder about the wisdom of mountain biking or any other relatively dangerous activity at middle age. Actually, I wonder about it at all ages. I blew out my knee playing ultimate frisbee at the age of 22 and crushed my shoulder in a skiing accident at the age of 50 – a crash that almost broke my pelvis as well, according to the orthopedist who saw me in the Vail ER following the accident. We live at a time when medicine can patch us up pretty well, but the consequence is that we are willing to take more risks with out bodies because they can be patched up. Not sure if that’s such a good thing! I do not think I will go skiing again – and will try to stick to activities from here on that make sense given the appreciable increase in frailty that inevitably comes with age. Other opinions may differ! Good luck with your recovery!
I enjoyed running and its relative safety for many years until my orthopedic surgeon told me to stop if I planned to be walking in 20 years. Then it was back to cycling only.
Jack LaLanne at the age of 80:
He was pretty impressive. But the activities he did were not risky in the same way that, say, free running is – activities that I think exist today because the consequences of an accident aren’t what they used to be. However, the clip is interesting to me because I ended up with afib at 45 after 38 years of routing aerobic exercise – exercise that was enough to increase my risk for afib by a factor of 5 over a normal population. So I feel like I made a mistake even though I was trying to be healthy. LaLanne took the same risk I guess, but he was not unlucky!
My AF started at the age of 57, after about 40 years of moderate weight training. (Not like Jack!)
It seems that genes have a lot to answer for.
We’re all different, and it’s best to try to get to know ourselves.
There’s no one answer to “What’s the best life style?”
Ask instead, “What’s best for the likes of me — my parent’s child?”
It doesn’t help that much of the generalized advice we got back then was flat wrong.